ASPN Abstract: Evaluation of Safety and Efficacy of the Streamlined Technique vs the Standard Technique
Author— Dawood Sayed, MD Published July 22, 2021
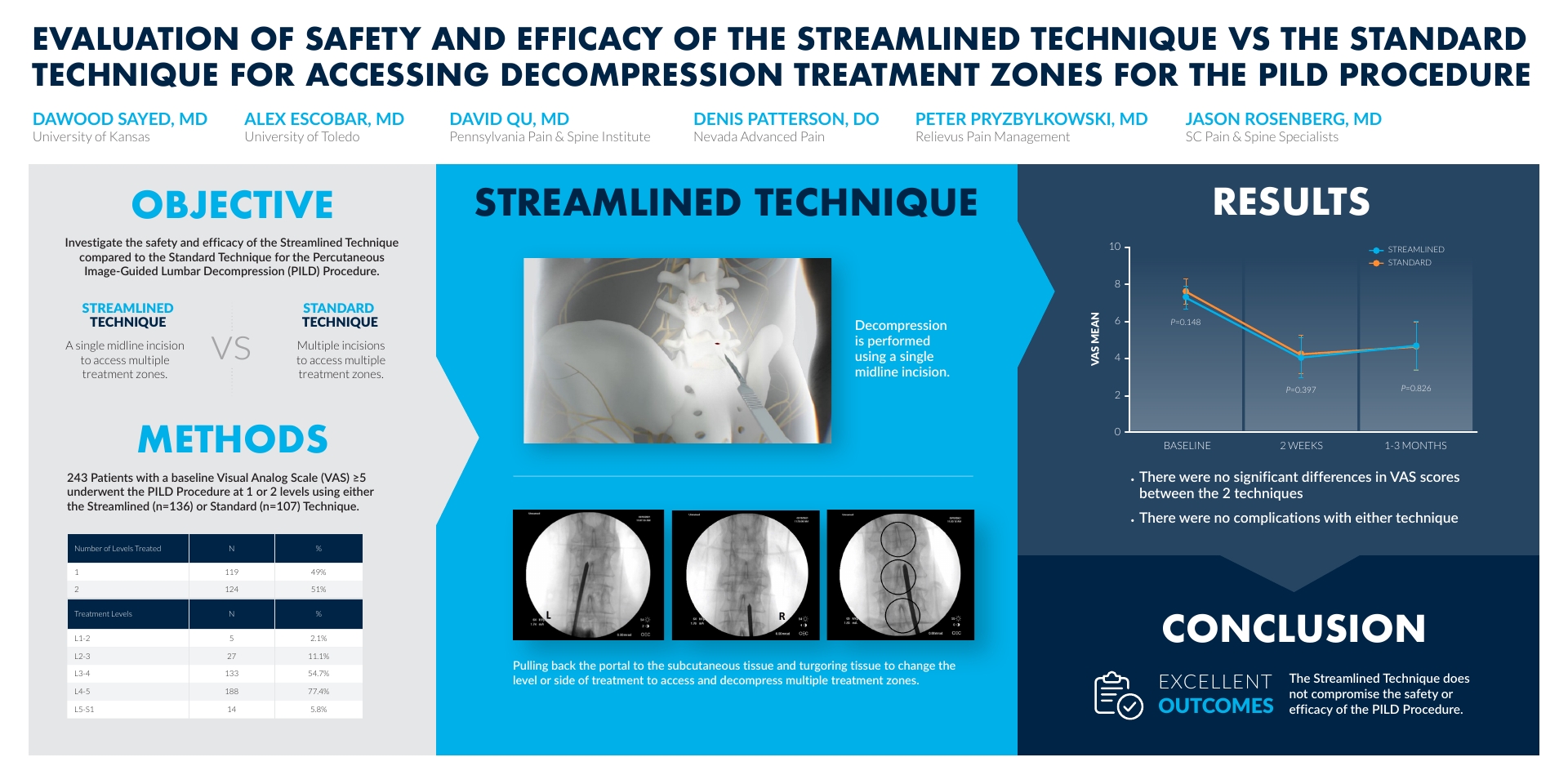
The following study, “Evaluation of Safety and Efficacy of the Streamlined Technique vs the Standard Technique for Accessing Decompression Treatment Zones for the PILD Procedure,” investigates the safety and efficacy of the Streamlined Technique compared to the Standard Technique. While the PILD, or mild® Procedure, may be performed using both methods, the Streamlined Technique enables a single midline incision to access multiple treatment zones whereas the Standard Technique uses one incision per treatment zone. The study involved 243 patients that underwent the mild® Procedure using either technique and tracked their outcomes. The authors concluded that the Streamlined Technique does not compromise the safety or efficacy of the mild® Procedure. View the abstract poster below to learn why the Streamlined Technique is an innovative approach to consider.
Watch Dr. Dawood Sayed present his abstract from the American Society of Pain and Neuroscience’s (ASPN) Third Annual Conference, where he discusses how the study found that adopting the Streamlined Technique allowed for efficient and effective decompression of multiple treatment zones, without compromising the safety or efficacy of the mild® Procedure.
Eager to further understand the mild® Procedure and the technique described above? Contact Vertos Medical to learn more about the Streamlined Technique or check out the animation and physician experience from Dr. Navdeep Jassal in this Procedure Evolution blog.
Dawood Sayed, MD (00:00)
Hello, I’m Dr. Dawood Sayed and I’m a Professor of Anesthesiology and Pain Medicine at the University of Kansas. Today on behalf of my co-investigators, I’m gonna be presenting our abstract, an “Evaluation of the Safety and Efficacy of the Streamlined Technique vs the Standard Technique for Accessing Decompression Treatment Zones for the Percutaneous Interlaminar Lumbar Decompression (PILD) Procedure.” Our objectives were to investigate the safety and efficacy of the Streamlined Technique compared to the Standard Technique for the percutaneous image guided lumbar decompressive procedure. In summary, the Streamlined Technique is a single midline incision to access multiple treatment zones versus the more traditional standard techniques, in which multiple incisions are made to access multiple treatments zones. It was the hypothesis of the investigators, that using the Streamlined Technique, that we would be able to perform the procedure in an equal satisfactory manner with the same efficacy, but also performing the procedure in a much less invasive manner for the patient.
(01:03) So our methods were 243 patients with a baseline visual analog score of greater than five. These patients underwent the PILD Procedure at 1 or 2 treatment levels using either the Streamlined Technique which is about 136 patients, or the Standard Technique, which was about 107 patients. If you look at the table here, you can see that most of the patients were treated at either the L-3, L-4 or the L-4, L-5 levels. And again, the Streamlined Technique is a decompression performed using a single midline incision. The technique involves pulling back the portal to the subcutaneous tissue, and triggering tissue to change the level or side of treatment, to access and decompress multiple treatment zones through a single incision. When we look at our results, you can see the average pain level was around an 8 on a VAS mean score. When you look at the immediate pain relief and efficacy at around 2 weeks, you can see that the difference between the results and efficacy between the Standard Technique and the Streamlined Technique was almost identical. When you look at these patients a little further out at 1 to 3 months, again, you can see no difference in the outcomes in pain scores, as well as complication rates between the two arms when comparing the Streamlined and Standard Technique. So in conclusion, the Streamlined Technique does not compromise safety or efficacy of the PILD Procedure. We look forward to evaluating this in a more prospective, rigorous manner, to evaluate it as a true change in the way we do this procedure. Thank you.
Benyamin RM, Staats PS, MiDAS ENCORE Investigators. mild® is an effective treatment for lumbar spinal stenosis with neurogenic claudication: MiDAS ENCORE Randomized Controlled Trial. Pain Physician. 2016;19(4):229-242.
Mekhail N, Costandi S, Abraham B, Samuel SW. Functional and patient-reported outcomes in symptomatic lumbar spinal stenosis following percutaneous decompression. Pain Pract. 2012;12(6):417-425. doi:10.1111/j.1533-2500.2012.00565.x.
2012 data from Health Market Sciences report for Vertos Medical 2013.
Data on file with Vertos Medical.
Staats PS, Chafin TB, Golvac S, et al. Long-term safety and efficacy of minimally invasive lumbar decompression procedure for the treatment of lumbar spinal stenosis with neurogenic claudication: 2-year results of MiDAS ENCORE. Reg Anesth Pain Med. 2018;43:789-794. doi:10.1097/AAP.0000000000000868.
Based on mild® Procedure data collected in all clinical studies. Major complications are defined as dural tear and blood loss requiring transfusion.
MiDAS ENCORE responder data. On file with Vertos Medical.
Jain S, Deer TR, Sayed D, et al. Minimally invasive lumbar decompression: a review of indications, techniques, efficacy and safety. Pain Manag. 2020;10(5). https://doi.org/10.2217/pmt-2020-0037. Accessed June 1, 2020.
Deer TR, Grider JS, Pope JE, et al. The MIST Guidelines: the Lumbar Spinal Stenosis Consensus Group guidelines for minimally invasive spine treatment. Pain Pract. 2019;19(3)250-274. doi:10.1111/papr.12744.
Hansson T, Suzuki N, Hebelka H, Gaulitz A. The narrowing of the lumbar spinal canal during loaded MRI: the effects of the disc and ligamentum flavum. Eur Spine J. 2009;18(5):679-686. doi:10.1007/s00586-009-0919-7.
Treatment options shown are commonly offered once conservative therapies (e.g., physical therapy, pain medications, chiropractic) are not providing adequate relief. This is not intended to be a complete list of all treatments available. Doctors typically recommend treatments based on their safety profile, typically prioritizing low risk/less aggressive procedures before higher risk/more aggressive procedures, but will determine which treatments are appropriate for their patients.
The mild® Procedure is a minimally invasive treatment for lumbar spinal stenosis. As with most surgical procedures, serious adverse events, some of which can be fatal, can occur, including heart attack, cardiac arrest (heart stops beating), stroke, and embolism (blood or fat that migrates to the lungs or heart). Other risks include infection and bleeding, spinal cord and nerve injury that can, in rare instances, cause paralysis. This procedure is not for everyone. Physicians should discuss potential risks with patients. For complete information regarding indications for use, warnings, precautions, and methods of use, please reference the devices’ Instructions for Use.
Patient stories on this website reflect the results experienced by individuals who have undergone the mild® Procedure. Patients are not compensated for their testimonial. The mild® Procedure is intended to treat lumbar spinal stenosis (LSS) caused by ligamentum flavum hypertrophy. Although patients may experience relief from the procedure, individual results may vary. Individuals may have symptoms persist or evolve or other conditions that require ongoing medication or additional treatments. Please consult with your doctor to determine if this procedure is right for you.
Reimbursement, especially coding, is dynamic and changes every year. Laws and regulations involving reimbursement are also complex and change frequently. Providers are responsible for determining medical necessity and reporting the codes that accurately describe the work that is done and the products and procedures that are furnished to patients. For this reason, Vertos Medical strongly recommends that you consult with your payers, your specialty society, or the AMA CPT regarding coding, coverage and payment.
Vertos Medical cannot guarantee coding, coverage, or payment for products or procedures. View our Billing Guide.
Vertos is an equal employment opportunity workplace committed to pursuing and hiring a diverse workforce. We strive to grow our team with highly skilled people who share our culture and values. All qualified applicants will receive consideration for employment without regard to sex, age, color, race, religion, marital status, national origin, ancestry, sexual orientation, gender identity, physical & mental disability, medical condition, genetic information, veteran status, or any other basis protected by federal, state or local law.
Hall S, Bartleson JD, Onofrio BM, Baker HL Jr, Okazaki H, O’Duffy JD. Lumbar spinal stenosis. Clinical features, diagnostic procedures, and results of surgical treatment in 68 patients. Ann Intern Med. 1985;103(2):271-275. doi:10.7326/0003-4819-103-2-271.
Kalichman L, Cole R, Kim DH, et al. Spinal stenosis prevalence & association with symptoms: The Framingham Study. Spine J. 2009;9(7):545-550. doi:10.1016/j.spinee.2009.03.005.
Fukusaki M, Kobayashi I, Hara T, Sumikawa K. Symptoms of spinal stenosis do not improve after epidural steroid injection. Clin J Pain. 1998;14(2):148-151. doi:10.1097/00002508-199806000-00010.
Mekhail N, Costandi S, Nageeb G, Ekladios C, Saied O. The durability of minimally invasive lumbar decompression procedure in patients with symptomatic lumbar spinal stenosis: Long-term follow-up [published online ahead of print, 2021 May 4]. Pain Pract. 2021;10.1111/papr.13020. doi:10.1111/papr.13020
Friedly JL, Comstock BA, Turner JA, et al. Long-Term Effects of Repeated Injections of Local Anesthetic With or Without Corticosteroid for Lumbar Spinal Stenosis: A Randomized Trial. Arch Phys Med Rehabil. 2017;98(8):1499-1507.e2. doi:10.1016/j.apmr.2017.02.029
Pope J, Deer TR, Falowski SM. A retrospective, single-center, quantitative analysis of adverse events in patients undergoing spinal stenosis with neurogenic claudication using a novel percutaneous direct lumbar decompression strategy. J Pain Res. 2021;14:1909-1913. doi: 10.2147/JPR.S304997
Pryzbylkowski P, Bux A, Chandwani K, et al. Minimally invasive direct decompression for lumbar spinal stenosis: impact of multiple prior epidural steroid injections [published online ahead of print, 2021 Aug 4]. Pain Manag. 2021;10.2217/pmt-2021-0056. doi:10.2217/pmt-2021-0056
Abstract presented at: American Society of Pain and Neuroscience Annual Conference; July 22-25, 2021; Miami Beach, FL.
Mobility Matters: Low Back Pain in America, Harris Poll Survey, 2022. View data and full summary here.
Deer TR, Grider JS, Pope JE, et al. Best Practices for Minimally Invasive Lumbar Spinal Stenosis Treatment 2.0 (MIST): Consensus Guidance from the American Society of Pain and Neuroscience (ASPN). J Pain Res. 2022;15:1325-1354. Published 2022 May 5. doi:10.2147/JPR.S355285.

